I Almost Canceled My Eye Exam—Then the Doctor's Face Changed and I Realized My Vision Wasn't the Problem
I Almost Canceled My Eye Exam—Then the Doctor's Face Changed and I Realized My Vision Wasn't the Problem
The Morning Everything Looked Wrong
So there I was, stopped at a red light on my usual morning commute, when the traffic signal split into three separate images. Not blurry—actually split, like someone had copy-pasted it twice across my vision. I blinked hard. Rubbed my eyes. The images merged back together, but my hands were gripping the steering wheel so tight my knuckles went white. This wasn't the first weird thing that had happened with my vision lately, but it was definitely the scariest. I'd been telling myself for months that I just needed reading glasses, that turning fifty meant your eyes got worse, that everyone deals with this stuff. But sitting there watching the light turn green, I couldn't ignore it anymore. When I got to work, I didn't even take off my coat before I called the optometrist. The receptionist had an opening in three days. I took it. I hung up the phone with the appointment scheduled, and a small voice in my head whispered: what if it's already too late?
 Image by RM AI
Image by RM AI
The Symptoms I'd Been Ignoring
Here's the thing about symptoms that creep up slowly—you rationalize every single one. The occasional double vision? Well, I was tired. The headaches that came and went? Stress from work, obviously. That weird whooshing sound I'd hear when I laid down at night? Probably just my heartbeat or something. I'd started needing more light to read, but I mean, that's just aging, right? My friends were all complaining about the same thing. There were mornings I'd wake up with my pillow damp because my eyes had been watering during the night. I bought better pillows. Sometimes I'd feel this pressure behind my eyes, like someone was gently pushing on them from inside my skull. I switched to decaf. Looking back now, I can see how perfectly I'd explained away everything. Each symptom had its own little excuse, its own rational explanation. I never put them together because why would I? Looking back at my calendar, I realized the first symptom had appeared almost six months ago—and I'd done absolutely nothing about it.
 Image by RM AI
Image by RM AI
When the Doctor Stopped Smiling
Dr. Martinez was young and friendly, the kind of doctor who makes small talk while he works. 'Any vacation plans?' he asked while I read the eye chart. 'How's work going?' Standard stuff. Then he had me put my chin in that machine where they shine the light in your eyes, and everything changed. The casual chatter stopped. I heard him inhale sharply. The silence stretched out, and I could feel him staring through that machine at something inside my eye. 'Everything okay?' I asked, trying to sound casual, but my voice came out too high. He didn't answer right away. When he finally pulled back, his professional smile was gone. His eyebrows were drawn together, and he was already reaching for a different instrument. 'Just want to get a better look at something,' he said, but his tone was completely different now. The friendly vacation-planning doctor had vanished. He pulled away from the machine and said quietly, 'I need to run another test,' and I felt my stomach drop.
 Image by RM AI
Image by RM AI
The Question That Changed Everything
Dr. Martinez rolled his chair closer to me, and I noticed he'd pulled out a notepad. That seemed bad. Doctors don't take notes during routine eye exams, do they? 'I'm seeing some changes that concern me,' he said carefully. 'I need to ask you some questions.' His pen was poised over the paper. 'Have you been experiencing headaches?' Oh God, yes. I started listing them—the morning ones, the ones that got worse when I bent over, the pressure behind my eyes. His pen was moving fast. 'Any nausea?' Sometimes, especially with the bad headaches. 'Vision changes beyond what you mentioned on the phone?' The double vision, the occasional blurriness, the way bright lights seemed too bright lately. 'That whooshing sound in your ears—can you describe it more?' Wait, how did he know about that? I hadn't mentioned it. With each answer, his expression grew more serious. He was connecting dots I didn't even know existed. When he asked if I'd had headaches, I started listing them—and watched his face grow more serious with every word.
 Image by RM AI
Image by RM AI
Telling James
James was making dinner when I got home, and I just stood in the kitchen doorway trying to figure out how to start the conversation. 'How was the eye appointment?' he asked, not looking up from the cutting board. 'Did you get a prescription?' I opened my mouth and nothing came out. He must have heard the silence because he turned around, knife still in hand. 'What's wrong?' So I told him. About the doctor's face changing, about all the questions, about how Dr. Martinez had made some calls while I waited and gotten me an emergency referral for imaging. 'Imaging? Like an MRI?' James put down the knife. 'For an eye exam?' His voice was steady, but I could see his jaw tighten. I watched him process it, watched him try to stay calm for me. He crossed the kitchen and pulled me into a hug. 'Okay,' he said into my hair. 'We'll figure this out.' James asked what the doctor said it could be, and I realized I had no idea—only that I needed imaging done tomorrow.
 Image by RM AI
Image by RM AI
The Internet Rabbit Hole
I know you're not supposed to Google symptoms. Every doctor tells you not to. James had gone to bed, but I sat there with my laptop, promising myself I'd just look for five minutes. Just to understand what could cause the things Dr. Martinez had seen. I typed in 'optic nerve swelling headaches double vision.' The results loaded. Then I made the mistake of clicking. Suddenly I was drowning in medical terminology I didn't understand. 'Papilledema.' 'Increased intracranial pressure.' Every article seemed to branch into more frightening possibilities. Brain tumors. Aneurysms. Strokes. Some websites showed before-and-after pictures of optic nerves. I stared at the swollen, damaged ones, wondering if that's what mine looked like. My chest got tight. One page led to another, then another. The words started blurring together, but one kept appearing in article after article, link after link. I'd hover my mouse over those links, then pull away. Every search led to the same word appearing again and again, and I couldn't bring myself to click on those links.
 Image by RM AI
Image by RM AI
The Waiting Room
The imaging center waiting room was packed with people, all of us trying not to look at each other. The woman across from me kept checking her phone, leg bouncing constantly. An older man sat perfectly still, hands folded in his lap, eyes closed. I wondered what they were here for. What invisible things were happening inside their bodies. We were all just waiting to find out if our lives were about to change. The receptionist called people back one by one, and the room got quieter with each name. I'd filled out the paperwork with shaking hands—medical history, current symptoms, emergency contact. There was a question about claustrophobia. I'd checked 'no,' but now I wasn't sure. My phone buzzed with a text from James: 'You've got this.' Did I though? A mother and teenage daughter sat together, holding hands. The daughter was crying softly. This was real life happening all around me, everyone carrying their own private terror. When they called my name, my hands were shaking so badly I could barely sign the consent forms.
 Image by RM AI
Image by RM AI
Inside the Machine
They gave me earplugs and a panic button, which somehow made everything feel more ominous. Dr. Patel, the radiologist, explained the procedure in a calm, rehearsed way that I'm sure was meant to be reassuring. The table slid me into the tube, and suddenly the world became this tight, humming tunnel. The machine started its banging rhythm—loud, mechanical, relentless. I tried to focus on breathing, on staying still, on not thinking about what they might find. Each sequence felt endless. BANG BANG BANG, then a pause, then different sounds. WHIRRRR. CLICK CLICK CLICK. I counted ceiling tiles I couldn't see, recited song lyrics in my head, anything to pass the time. They'd said twenty minutes. It felt like hours. Then the machine went quiet. I thought we were done. Relief started flooding through me. The technician's voice came through the speaker: 'We need a few more images,' and I knew that wasn't part of the standard protocol.
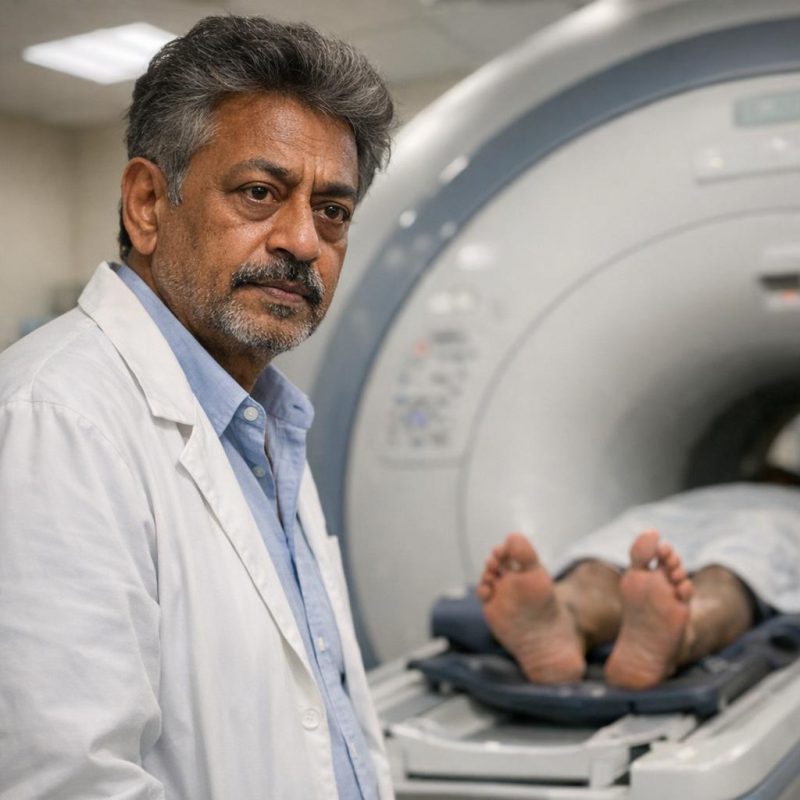 Image by RM AI
Image by RM AI
The Friend Who Knew
I texted Lisa that night because I couldn't hold it in anymore. We'd been friends since college—she was the person I called when life got messy. She came over with wine she knew I probably shouldn't drink and sat across from me at my kitchen table. 'I've been trying to convince myself it's nothing,' I told her, and she just nodded. Lisa had her own health scare two years ago, something with her thyroid that turned out okay after months of tests and worry. 'You know what helped me?' she said. 'Remembering that most of the terrible things I imagined didn't actually happen.' I wanted to believe her. We talked for hours, crying a little, laughing at inappropriate moments the way you do when everything feels fragile. She shared details about her appointments, the waiting rooms, the terror of not knowing. It helped to hear someone else had walked through this fog and come out the other side. But then she got quiet, looking down at her wine glass. Lisa said, 'The worst part isn't the diagnosis—it's the not knowing,' and I realized I was about to find out which was actually worse.
 Image by RM AI
Image by RM AI
The Call
Dr. Martinez called my cell two days later, which itself felt wrong—doctors don't usually call personally unless it matters. I was at the grocery store, standing in the cereal aisle, and suddenly the fluorescent lights felt too bright. 'Karen, we got your MRI results back,' he said, his voice careful in that way that made my stomach drop. He explained there was evidence of increased pressure around the optic nerve, that this needed urgent attention from a specialist. I asked him what it meant, and he gave me that professional deflection: 'I want you to see someone who specializes in this before we jump to conclusions.' Then he used the word 'urgent' to describe the appointment he was arranging. I asked when, and he said 'urgent' again. The specialist could see me in three days, which he called 'urgent' a third time. I stood there holding a box of cereal I didn't remember picking up, people moving around me doing normal grocery shopping while my world tilted sideways. He said 'urgent' three times in one conversation, and by the third time, I couldn't hear anything else he was saying.
 Image by RM AI
Image by RM AI
The Sleepless Night
That night, sleep was impossible. James fell asleep around eleven, his breathing steady beside me while I stared at the ceiling. Every time I closed my eyes, my mind spun through scenarios—surgery, blindness, worse things I didn't want to name. I googled symptoms at 1 AM, which everyone knows you should never do, but I couldn't stop myself. The internet offered a thousand terrible possibilities. James stirred when I got up to pace around 2 AM. 'Come back to bed,' he mumbled, half-asleep. I tried. I really did. But lying there in the dark, I kept thinking about all the ordinary moments I'd taken for granted—reading books, seeing my nephew's face, watching sunsets. Stupid things that suddenly felt precious. I thought about my job, my unfinished projects, places I'd always meant to visit. The rational part of my brain knew I was catastrophizing, that I didn't even have a diagnosis yet. But the scared part didn't care about rational. At 3 AM, I started making a mental list of everything I still wanted to do, and that's when I knew I'd crossed into a darker kind of fear.
 Image by RM AI
Image by RM AI
Meeting Dr. Chen
Dr. Chen's office was in a different medical building, one of those modern places with abstract art that's supposed to be calming. James came with me because I'd asked him to, because I knew I might not remember everything she said. Dr. Chen was younger than I expected, efficient without being cold. She shook both our hands and got right to business, which I appreciated—I couldn't handle more small talk about the weather. She asked detailed questions about my symptoms, writing notes in quick, precise handwriting. Then she logged into her computer and pulled up my scans. I'd never actually seen them before. There was my brain, my skull, everything that made me who I was, reduced to gray-and-white images on a screen. She used her pen to point at areas, explaining what she was seeing. The images looked alien to me, incomprehensible. Dr. Chen pulled up my scans on the screen, pointed to a bright spot behind my left eye, and said, 'This is what we're dealing with.'
 Image by RM AI
Image by RM AI
What Pressure Means
The bright spot, Dr. Chen explained, wasn't a mass exactly—it was swelling, evidence of pressure building where it shouldn't be. She drew diagrams showing how the optic nerve connects to the brain, how pressure in that area could damage the nerve fibers. 'Think of it like a garden hose,' she said. 'If something presses on it, the flow gets restricted.' Except this wasn't water—it was signals from my eye to my brain, the connection that let me see. She talked about intracranial pressure, about how the space inside the skull is fixed and unforgiving. James asked the question I was too scared to: what happens if the pressure continues? Dr. Chen didn't sugarcoat it. Optic nerve damage is progressive, she said. Vision loss can be gradual or sudden. Some of it might be reversible if caught early. Some might not be. She said the word 'permanent' twice—permanent vision loss, permanent damage—and I realized I might already be out of time.
 Image by RM AI
Image by RM AI
The Differential Diagnosis
Dr. Chen pulled out a notepad and started listing possibilities. Idiopathic intracranial hypertension—pressure without a clear cause. Venous sinus thrombosis—a blood clot affecting drainage. Inflammatory conditions affecting the meninges. Structural abnormalities. And yes, she said, they also needed to rule out masses or lesions. My breath caught on that last one. James reached for my hand. 'We need more information before we can determine what we're dealing with,' Dr. Chen said. Some conditions were manageable with medication, she explained. Others required surgery. Some resolved on their own. Others didn't. I asked her which one she thought it was, and she gave me an honest answer I didn't want: 'I don't know yet.' She explained that each possibility had different markers, different tests, different treatment protocols. We needed to be methodical, she said. Systematic. But all I heard was uncertainty, weeks or months of not knowing while something pressed against my optic nerve. The list of possibilities ranged from treatable to terminal, and we wouldn't know which until more tests came back.
 Image by RM AI
Image by RM AI
The Blood Work
The lab was in the basement of the medical complex, fluorescent and sterile. The phlebotomist who called my name was young, probably early twenties, with kind eyes above her mask. Her name tag said Rachel. 'Lots of tubes today,' she said apologetically, arranging them in a rack. I asked what they were testing for, and she rattled off a list: inflammation markers, clotting factors, autoimmune panels, thyroid function, vitamin levels, infection markers. It sounded like they were casting the widest possible net. Rachel was good at her job—I barely felt the needle. But watching vial after vial fill with dark red blood was surreal. Each one got a different colored cap, a different label. She lined them up carefully, methodically. 'Fourteen,' she said when she finally pressed the gauze to my arm. Fourteen vials. I stared at them, all that blood holding potential answers. Dr. Chen wanted a complete picture, Rachel explained. These tests would help narrow down the differential diagnosis. I nodded like I understood, but really I was just stunned. The phlebotomist filled fourteen vials, and I wondered what they were looking for in my blood that the scans couldn't show.
 Image by RM AI
Image by RM AI
Telling Work
Calling my boss felt impossible, but I couldn't put it off any longer. I'd already missed two days for appointments, and Dr. Chen had made it clear there would be more—many more. I closed my office door and dialed, rehearsing what to say. How do you explain something you don't understand yourself? 'I need to take medical leave,' I said when he answered. 'There's a situation with my vision, and the doctors need to run more tests.' The silence on the other end lasted too long. He asked if it was serious. I said I didn't know yet, which was the truth but sounded evasive. He asked about my projects, the timeline, who would cover for me. Normal boss questions that felt absolutely unimportant compared to potentially going blind, but I understood he had to ask. 'Of course, take whatever time you need,' he finally said, his voice shifting into sympathetic mode. 'Just keep us posted.' Then came the question I'd been dreading. My boss asked when I'd be back, and I had to say I honestly didn't know—which made it all feel even more real.
 Image by RM AI
Image by RM AI
The Side Effects Start
The headaches started waking me up at night. Not every night at first—just once or twice a week—but then it became regular. I'd lie there in the dark, feeling the pressure build behind my eyes like someone was slowly inflating a balloon inside my skull. The floaters were worse too, these dark shadows that drifted across my vision whenever I looked at anything bright. I tried to tell myself it was just because I was paying attention now, that I'd always had these symptoms and hadn't noticed. Maybe the eye doctor had just made me hyperaware of normal things. But deep down, I knew that wasn't true. The pressure was real. The pain was real. I started keeping a journal, documenting every symptom, every headache, every weird visual thing that happened. I thought maybe if I tracked it all, I could prove to myself—or to the doctors—that something was actually changing. Or maybe I was just trying to maintain some sense of control when everything felt like it was spiraling. The headaches were getting worse, and I couldn't tell if it was the pressure increasing or just my awareness of it.
 Image by RM AI
Image by RM AI
The Support Group
Lisa called me three times before I finally answered. 'You need to talk to someone who understands,' she said. 'I found this online support group for people with vision issues.' I didn't want to. The last thing I needed was to hear horror stories from strangers on the internet. But she wore me down, and honestly, I was desperate for something—anything—that might help me feel less alone. The group met on Zoom twice a week. There were maybe eight people on the call that first night, ranging from early twenties to seventies. Some had glaucoma, others had conditions I'd never heard of. They were kind, welcoming even. A few shared stories of successful treatments, stable vision, normal lives. That part helped. But then this woman, probably in her thirties, started talking about her rapid progression. How she'd gone from normal vision to legally blind in less than a month. How the doctors couldn't stop it despite trying everything. I felt my chest tighten. My hands went numb. One woman shared her story of going blind in three weeks, and I had to leave the call because I couldn't breathe.
 Image by RM AI
Image by RM AI
What I Should Have Said
I couldn't sleep after that support group call, so I did something I'd been avoiding. I logged into the patient portal and started going through my medical records from the past few years. All those times I'd complained about headaches to my primary care doctor. The weird visual disturbances I'd mentioned during routine checkups. The fatigue I thought was just getting older. It was all there, documented in clinical notes that made my blood boil. 'Patient reports increased stress at work.' 'Anxiety likely contributing to physical symptoms.' 'Recommended relaxation techniques and better sleep hygiene.' One note from eighteen months ago actually documented that I'd described seeing floaters and experiencing pressure headaches. The doctor's assessment? 'Consistent with tension headaches. Patient encouraged to manage stress levels.' No tests ordered. No referrals made. Just a prescription for anxiety that I never filled because I wasn't anxious—I was sick. I found my medical records from two years ago where I'd complained about headaches and visual changes, and the notes just said 'patient reports stress.'
 Image by RM AI
Image by RM AI
The Neurosurgeon
Dr. Kowalski's office was in a different building, one that felt more serious somehow. James came with me because I'd started bringing him to all my appointments—I couldn't trust myself to remember everything anymore. The neurosurgeon was older, maybe sixty, with gray hair and steady hands that he kept perfectly still while he talked. He explained that if the medication didn't reduce the intracranial pressure, surgery might become necessary. Not might—would. He showed us diagrams of the procedure, pointing to where they'd need to go in. Something about creating a shunt to drain excess cerebrospinal fluid. His voice was calm, professional, like he was describing how to change a tire instead of drilling into someone's skull. James asked about risks. Dr. Kowalski listed them: infection, bleeding, need for revision surgery. All said in that same measured tone. I appreciated that he didn't sugarcoat it, but I also hated how routine it sounded to him. He explained the surgery with calm precision, and all I could think was: he's done this before, which means other people have needed their skull opened for this.
 Image by RM AI
Image by RM AI
The Medication Trial
Dr. Chen called me back to her office two days after the neurosurgeon consultation. She wanted to start me on medication immediately—a diuretic called acetazolamide that would hopefully reduce the fluid pressure around my brain. 'We're not waiting for all the test results,' she said. 'Your pressure numbers are high enough that we need to intervene now.' She explained how the medication worked, how it would help my body eliminate excess cerebrospinal fluid. Then came the side effects list. Tingling in my hands and feet. Frequent urination. Possible nausea. Fatigue. Metallic taste in my mouth. Carbonated drinks would taste flat. The list went on. I signed the prescription authorization form without hesitation. She handed me the pharmacy information and told me to start that evening. 'Call me if the side effects become unbearable,' she said. 'But give it at least a week before we consider switching.' I nodded, clutching the prescription. She warned me about side effects, but I would have taken anything if it meant keeping my vision—I just didn't realize how hard 'anything' would be.
 Image by RM AI
Image by RM AI
When the Cure Feels Worse
The tingling started within an hour of my first dose. Just a weird pins-and-needles sensation in my fingers that I could ignore. By day two, my feet felt numb and everything tasted like I'd been sucking on pennies. By day three, the nausea hit like a truck. I couldn't keep anything down—not toast, not crackers, not even water. James found me on the bathroom floor at two in the morning, sweating and shaking. 'Maybe you should stop taking it,' he said, holding my hair back. I shook my head. The thought of going blind was worse than anything this medication could do to me. I took the next dose at six AM despite feeling like death. And the one after that. The tingling spread up my arms. Food tasted like metal and cardboard. I peed every thirty minutes. I couldn't drink my morning coffee because it tasted wrong. Everything felt wrong. I spent three hours throwing up, and James asked if I was sure I should keep taking it, but I thought about going blind and reached for the next dose.
 Image by RM AI
Image by RM AI
The First Follow-Up
The follow-up appointment was scheduled for two weeks after starting the medication. I'd lost eight pounds because I could barely eat. My hands still tingled constantly. But I'd kept taking it, every single dose, because that's what Dr. Chen had told me to do. She did another eye pressure measurement, the same uncomfortable procedure as before. Then she had me do some visual field tests on the computer, clicking whenever I saw a flash of light. I tried to read her expression while she reviewed the results, but she had that perfect doctor poker face. No frowns, no smiles, just professional neutrality. 'The pressure is slightly lower,' she finally said. Slightly. Not significantly. Not dramatically. Just slightly. 'We'll continue the current dose for another month and recheck.' I asked if that meant it was working. She said it meant we were seeing some response, but it was too early to know if it would be enough. Too early to know if I was poisoning myself for nothing. Dr. Chen measured the pressure in my eye and her face didn't change, which somehow felt worse than if she'd looked worried.
 Image by RM AI
Image by RM AI
Sarah's Story
Sarah showed up at my door on a Thursday afternoon with two suitcases and a determined expression I recognized from childhood. 'I took a leave from work,' she announced. 'You need help and I'm staying.' I tried to protest, but honestly, I was relieved. James had been amazing, but he still had to work, and I was struggling with basic things like grocery shopping and cooking. Sarah took over my kitchen, made me actual meals I could stomach, drove me to appointments. One night, about a week into her stay, we were doing dishes together when she suddenly said, 'I had a breast cancer scare last year.' I nearly dropped the plate I was holding. She'd never mentioned it. Nobody in the family knew. 'I found a lump,' she continued. 'Spent two months in testing hell before they confirmed it was benign. And I didn't tell anyone because I thought I should be strong enough to handle it alone.' She looked at me then, really looked at me. Sarah said, 'I didn't tell anyone because I thought I could handle it alone,' and I realized I'd been doing exactly the same thing.
 Image by RM AI
Image by RM AI
The Inflammation Markers
Dr. Chen called me at home two days after my latest round of bloodwork, which was never a good sign. 'Some of your inflammatory markers are elevated,' she said, her voice careful in that way doctors use when they're not entirely sure what they're looking at yet. I had no idea what inflammatory markers even were. She explained that certain proteins in my blood suggested my immune system was reacting to something, that there might be an autoimmune component we hadn't considered. 'I'm referring you to a rheumatologist,' she continued. 'Dr. Patel is excellent. She'll help us figure out if there's a connection.' I sat there holding the phone, trying to process this new direction. We'd been focused on my eyes, on pressure and tumors and medication adjustments. Now we were talking about my immune system attacking itself? It felt like every appointment opened a new door to something worse, like playing the world's most terrifying version of medical whack-a-mole. I wrote down Dr. Patel's name with shaking hands. Dr. Chen said the inflammation could be significant, and scheduled me with a rheumatologist, which opened up a whole new category of terrifying possibilities.
 Image by RM AI
Image by RM AI
Losing Time
I started keeping track in a notebook, just to see the pattern in black and white. Three ophthalmology appointments. Two MRIs. Bloodwork drawn five times. The rheumatology consultation coming up. Follow-up calls with Dr. Chen. Hours in waiting rooms scrolling through my phone, trying not to think about what they might find. Hours lying still in machines. Hours talking to receptionists about insurance pre-approvals. I'd taken more sick days in three weeks than I'd taken in the past three years combined. My supervisor was understanding, but I could hear the strain in her voice when I called in again. My projects were piling up, reassigned to colleagues who were already overloaded. I used to pride myself on being reliable, the person who never missed deadlines. Now I was the person whose calendar was color-coded by which specialist I was seeing. I used to have a life outside doctor's offices. I used to make dinner plans and actually keep them. I looked at my calendar and realized I'd spent more time in hospitals in the past three weeks than I had in the previous ten years combined.
 Image by RM AI
Image by RM AI
The Medication Adjustment
Dr. Chen pulled up my latest pressure readings on her computer screen, and I could tell from her expression it wasn't what she'd hoped for. 'The medication isn't controlling it as well as I'd like,' she said. 'I want to increase your dosage.' I knew what that meant. The current dose already made me feel like I was wading through fog, gave me headaches, made my hands tingle at odd moments. Doubling it would double all of that. But what choice did I have? We were trying to save my vision. That was worth feeling like garbage for a few weeks, worth the brain fog and the fatigue and whatever other side effects came along for the ride. 'Okay,' I said, and my voice sounded steadier than I felt. She handed me the new prescription, went over the dosage instructions again, reminded me to call if the side effects became unbearable. I nodded, folded the paper, put it in my purse. I was already mentally preparing myself for how the next few weeks would feel. She doubled the dose and I didn't argue, even though I knew what that meant for how I'd feel for the next few weeks.
 Image by RM AI
Image by RM AI
The Things I Took for Granted
That night, I couldn't sleep, so I made a list in my head of everything I'd never really noticed before. The way morning light hits the kitchen counter. The individual leaves on the tree outside our bedroom window. The expression on James's face when he's concentrating on something. The titles of books on our shelves. My own handwriting. The smile lines around Sarah's eyes. I'd spent forty-nine years seeing without really seeing, taking it all for granted the way you take breathing for granted until you can't. Now every visual detail felt precious, something I needed to memorize and store away. I found myself staring at ordinary things—the pattern on our living room rug, the photographs on the wall, the way shadows moved across the ceiling. James came to bed around midnight and found me just lying there in the dark. 'Can't sleep?' he asked, and I shook my head. He settled in beside me, and I turned to look at him in the dim light from the hallway. I watched James across the room and tried to memorize his face, just in case.
 Image by RM AI
Image by RM AI
The Rheumatology Appointment
Dr. Patel's office was in a different medical building, one I'd never been to before. She was younger than I expected, thorough in a way that felt both reassuring and exhausting. She asked about my current symptoms, then started going backward. 'Any joint pain in the past few years?' Yes, actually, in my knees and hands, but I'd assumed that was just getting older. 'Unexplained fatigue?' God, yes, but who isn't tired? 'Headaches?' I'd been having them for years, dismissed by three different doctors as tension or stress. 'Sensitivity to light?' Sometimes, I admitted. She kept writing, kept asking, going back through my medical history like she was mining for gold. Things I'd mentioned to doctors before, things that had been brushed off as normal or stress-related or just part of being a woman in her forties. Suddenly they were all on the table again, being examined under a different lens. The rheumatologist asked about my medical history going back years, and patterns started emerging that I'd never connected before.
 Image by RM AI
Image by RM AI
Michael's Visit
Michael came home on Friday, and I wasn't prepared for how much it would hurt to see the worry on his face. He's twenty-five, supposed to be focused on his graduate program and his girlfriend and his own life. Not on whether his mother is going to go blind. James picked him up from the train station, and when they walked through the door, Michael tried to act casual, but I saw how his eyes scanned my face, looking for signs of how bad things really were. We ordered pizza, tried to keep conversation light, but eventually he just asked directly. 'How serious is this, Mom?' I'd been honest with him from the start, refusing to sugar-coat or minimize. But sitting there looking at my son, I realized honesty without hope is just cruelty. 'It's serious,' I said. 'But we're figuring it out. The doctors are good. We're getting answers.' He nodded, but his jaw was tight. He asked if I was going to be okay, and I realized I'd been so focused on being honest that I forgot he needed hope too.
 Image by RM AI
Image by RM AI
The Second MRI
The second MRI was scheduled for a Tuesday morning, and this time I knew what to expect. The same changing room, the same gown, the same technician explaining what would happen even though I'd done this before. I lay down on the sliding table, fitted the same panic button into my hand, let them position my head in the cradle. The machine swallowed me up again with those same loud clanging sounds, the same rhythm of mechanical breathing. But something was different this time. I wasn't afraid. I was just... done with not knowing. Done with the waiting and the wondering and the endless speculation about what might be happening inside my skull. If there was something growing in there, I wanted to know. If the pressure had gotten worse, I wanted to know. If the treatment was working or failing, I wanted to know. Any answer felt better than this limbo. The machine banged and hummed around me, and I kept my eyes closed and my breathing steady. This time in the machine, I wasn't afraid—I was just tired of not knowing, and ready for any answer they could give me.
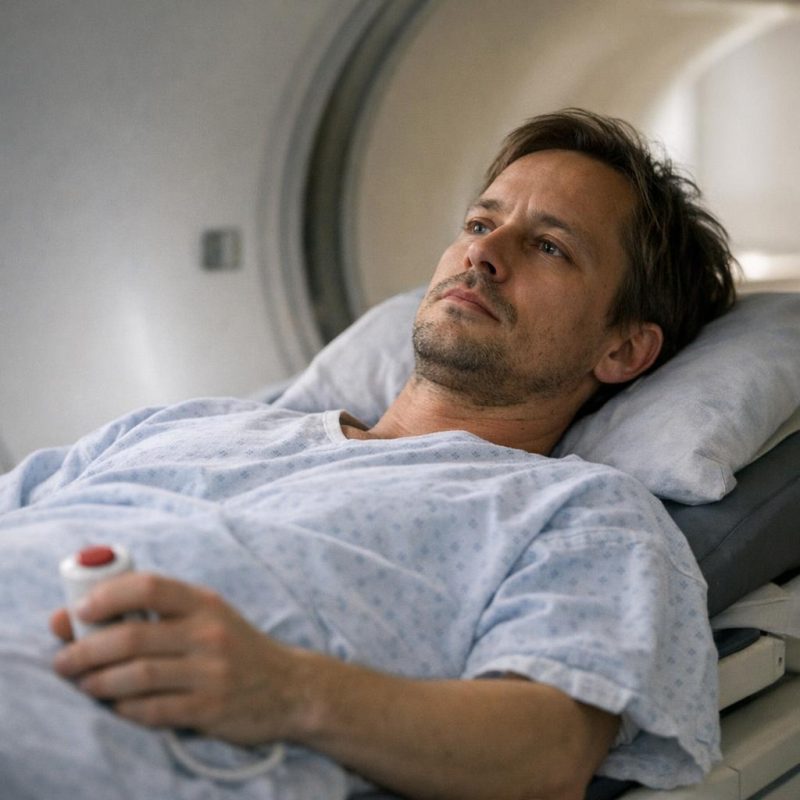 Image by RM AI
Image by RM AI
Comparing the Scans
Dr. Chen pulled up both MRI images on her dual monitors, the before and after displayed side by side. I leaned forward, trying to see what she was seeing, looking for obvious differences. 'The good news,' she started, and I braced myself because sentences that start that way always have a 'but' coming. 'The good news is there's no growth. No tumor. And the pressure hasn't gotten significantly worse.' I waited for the other shoe to drop. 'But it also hasn't improved. Despite the medication increase, despite everything we've tried, the pressure is essentially unchanged.' I stared at the images, at the identical-looking black and white swirls that supposedly held the answer to why my vision was at risk. We'd been throwing medication at this problem for weeks now. I'd been dealing with side effects, taking pills multiple times a day, and apparently it hadn't made a damn bit of difference. She said 'stable' like it was good news, but all I heard was that nothing we were doing was actually working.
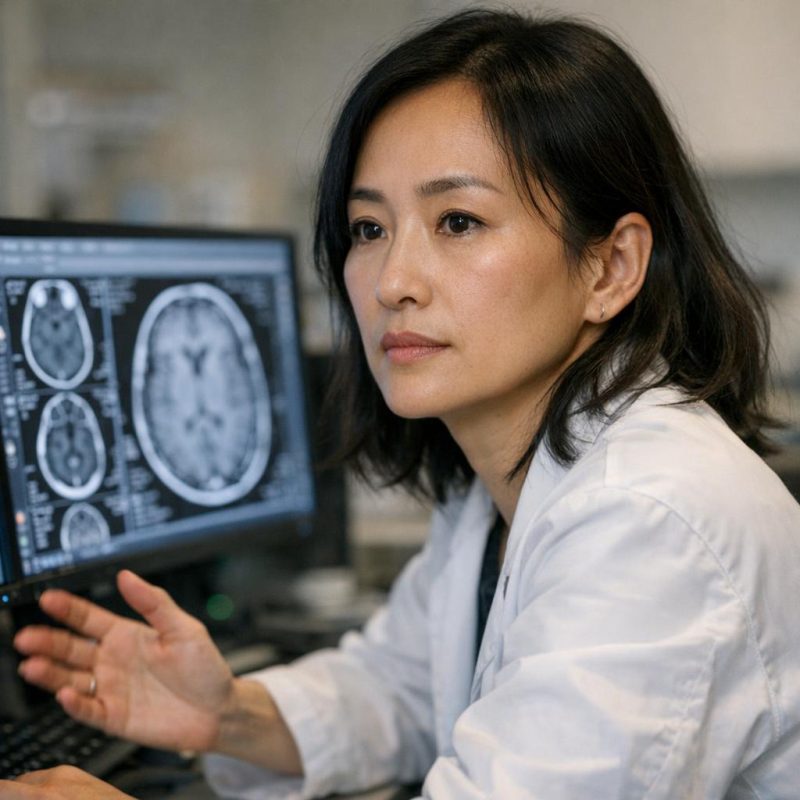 Image by RM AI
Image by RM AI
The Tumor Question
Dr. Chen must have seen something shift in my face because she leaned back slightly, giving me space to process. 'I know this feels like we're not getting anywhere,' she said, 'but the fact that nothing has changed—no growth, no new findings—is actually encouraging in its own way.' I tried to understand how 'nothing changing' could be good when my vision was still at risk. 'A tumor would show progression. We'd see expansion, infiltration, changes in the surrounding tissue.' She pointed to different areas on the screen, but honestly, it all looked the same to me. 'The stability suggests we're dealing with something else, something more manageable once we identify it.' The word 'tumor' was starting to feel less heavy in the room, which should have been a relief. I should have been celebrating that we were ruling out the worst-case scenario. But instead, I just felt more lost. If it wasn't a tumor, what the hell was it? Why was my brain under so much pressure? Why weren't the medications working? She said the word 'tumor' felt less likely now, which should have been relief, but instead I just felt more confused about what we were actually fighting.
 Image by RM AI
Image by RM AI
The Specialist Panel
The next part caught me completely off guard. Dr. Chen pulled up what looked like a calendar on her computer and started scrolling through appointment slots. 'I'm presenting your case to our multidisciplinary team next Thursday,' she said, like this was a routine thing. 'We do these case reviews when we have patients who don't fit typical patterns.' I didn't know whether to feel special or terrified. On one hand, it meant she was taking me seriously, that she wasn't just dismissing my symptoms or giving up. On the other hand, it meant I was complicated enough to require a panel of specialists to weigh in. 'It'll be neurologists, ophthalmologists, endocrinologists, radiologists—basically anyone who might catch something we're missing,' she explained. I nodded, trying to look grateful, which I was. But I also felt like I was becoming less of a person and more of a puzzle to be solved. A teaching moment. An interesting abnormality. Dr. Chen said, 'We want more eyes on this,' and I wondered if being an interesting case was better or worse than being a straightforward one.
 Image by RM AI
Image by RM AI
The Anxiety Attribution
That night, I couldn't sleep. I pulled out all my old medical records—years of them, stuffed in a filing box I'd shoved in the back of my closet. I started going through every visit, every complaint I'd brought to doctors over the past decade. And there it was, a pattern I'd somehow normalized. 2014: 'Patient reports headaches and fatigue. Discussed stress management and sleep hygiene.' 2016: 'Continues to experience headaches. Anxiety appears to be primary concern.' 2018: 'Patient tearful, reports overwhelming fatigue. Recommended counseling for anxiety and depression.' 2019: 'Persistent headaches, patient appears anxious. Discussed relaxation techniques.' 2021: 'Patient reports visual disturbances, headaches. Anxiety assessment completed.' Every single time, the conclusion was the same: it's in your head, but not the way you think. It's stress. It's anxiety. It's being a busy woman in her forties. Not one of them had ordered a scan. Not one had suggested there might be a physical cause. Five different doctors, five different years, all saying the same thing: it's just stress—and none of them had been right.
 Image by RM AI
Image by RM AI
The Fatigue No One Believed
The fatigue was what really got to me as I sat there with those records spread across my dining room table. I'd been so tired for so long that I'd forgotten what normal energy felt like. There were years when getting through a workday felt like climbing a mountain. I'd come home and collapse on the couch, unable to do anything else. My friends would invite me out and I'd decline, again and again, until they stopped asking. Everyone had an explanation: you work too much, you need to exercise more, you're not getting enough sleep, you're getting older, maybe you need vitamins, have you tried meditation? I'd tried everything. I bought a Fitbit, joined a gym, took B12 supplements, cut out caffeine, downloaded sleep apps. Nothing helped. And the whole time, people kept telling me it was normal. That everyone's tired. That this is just what forty-something feels like. I'd believed them. I'd believed I was just weak, or lazy, or doing something wrong. I'd spent a decade being told I was just tired, and now I couldn't stop wondering: what if my body had been screaming at me the whole time?
 Image by RM AI
Image by RM AI
The Lumbar Puncture
The lumbar puncture was scheduled for the following week, and Dr. Patel himself would be doing it. I'd almost forgotten about him since that first urgent appointment, but apparently he'd been consulting with Dr. Chen all along. 'This will give us definitive pressure readings,' he explained as I lay curled on my side on the exam table. 'And we'll test the fluid itself for any signs of infection, inflammation, or abnormal cells.' The procedure itself wasn't as bad as I'd feared—a sharp pinch, some pressure, an odd sensation of something being where it shouldn't be. But the waiting while they measured was excruciating. I could hear them murmuring numbers, could feel the tension in the room shift. When Dr. Patel finally helped me sit up, his face was serious. 'Your opening pressure was 42 centimeters of water,' he said. I had no context for what that meant. 'Normal is 20 or below. 25 is considered elevated. You're at double the normal pressure.' My brain was being squeezed by fluid that had nowhere to go, and now we had proof. The pressure reading was twice what it should have been, and the neurologist said that number explained a lot—but not what was causing it.
 Image by RM AI
Image by RM AI
The Medication Failure
Dr. Chen called me two days after the lumbar puncture results came back. The fluid itself was clear—no infection, no cancer cells, no obvious inflammation. Which should have been good news, except we were running out of explanations. 'The medication clearly isn't controlling the pressure effectively,' she said, and I could hear the shift in her tone. We were moving into different territory now. 'We need to talk about more aggressive management options.' I sat down at my kitchen table, pen in hand, ready to take notes. 'There are surgical interventions we can consider. A VP shunt would drain excess fluid from your brain to your abdomen. It's a permanent solution for pressure management, though it comes with its own risks and maintenance requirements.' The word 'shunt' sounded so mechanical, so invasive. 'Or there's optic nerve sheath fenestration, which relieves pressure around the optic nerve specifically to protect your vision.' I was writing everything down, but my hand was shaking. We'd gone from 'try these pills' to 'let's cut into your skull' in what felt like no time at all. She mentioned words like 'shunt' and 'surgical intervention' while I sat there realizing we'd run out of easy options.
 Image by RM AI
Image by RM AI
The Weight Conversation
Before the surgical consult, I had to see one more specialist—an endocrinologist who wanted to rule out hormonal causes. He was older, probably close to retirement, and within five minutes of the appointment, I knew where this was going. 'Have you considered that weight loss might alleviate some of your symptoms?' he asked, barely looking up from his chart. There it was. I'd been waiting for it. 'There's a well-documented correlation between obesity and intracranial pressure,' he continued, launching into a speech I could have recited myself. I sat there, feeling my face get hot, feeling fourteen years old again, being weighed at the school nurse's office while other kids snickered. Feeling like every health problem I'd ever had was being reduced to a number on a scale. I'd lost weight before. I'd gained it back. I'd lost it again. Through all of it—thin, heavy, and everywhere in between—the headaches had persisted. The fatigue had persisted. But sure, let's blame my body instead of actually investigating what's wrong with it. I'd heard this speech before, from doctors who never looked deeper—and I was done pretending weight explained everything that was wrong with me.
 Image by RM AI
Image by RM AI
When I Started Keeping Score
That night, something in me snapped. I opened a new document on my laptop and started typing. Every symptom I could remember, going back as far as I could recall. Every doctor's visit where I'd been dismissed. Every time I'd been told it was anxiety, stress, or weight. Every time I'd left an appointment feeling smaller, crazier, more convinced I was making things up. The document grew. Three pages. Four. Headaches that started in my twenties. The whooshing sound in my ears that came and went for years. The fatigue that everyone said was normal. The visual changes I'd mentioned to my optometrist five years ago that he'd said were 'just aging.' The time I went to the ER with the worst headache of my life and they gave me Tylenol and sent me home. The pattern was so clear now that I couldn't believe I'd missed it. Or maybe I hadn't missed it. Maybe I'd been trained not to see it. Trained to doubt myself, to minimize, to accept whatever explanation I was given because doctors know best, right? The list was three pages long, and I realized I'd been gaslit by the medical system for so long that I'd started gaslighting myself.
 Image by RM AI
Image by RM AI
The Panel Results
Dr. Chen called me in for the panel results three days after their meeting. I'd spent that entire time in this weird limbo between hope and dread, trying not to obsess over what a multidisciplinary team meant when they 'couldn't reach consensus.' James had tried to reassure me that disagreement was good, meant they were being thorough, but I couldn't shake the feeling that I was becoming some kind of medical mystery nobody wanted to solve. When I sat down in her office, Dr. Chen had that careful expression doctors get when they're about to deliver news that isn't simple. 'The team reviewed everything,' she said. 'Your imaging, your symptoms, the progression. And the consensus is that this doesn't fit typical tumor patterns. The way your symptoms have evolved over years, the fluctuating nature of your headaches, the periods of remission—it's pointing us toward something else.' She pulled out a requisition form already filled with test names. 'We want to run a comprehensive autoimmune panel. There are several conditions that can cause increased intracranial pressure through immune system dysfunction.' Dr. Chen said they wanted to test for conditions I'd never heard of, and I didn't know whether to be hopeful that we might find answers or terrified of what those answers might be.
 Image by RM AI
Image by RM AI
The Autoimmune Alphabet
That night, I made the mistake of Googling every condition on the requisition form. Neurosarcoidosis. Behçet's disease. CNS vasculitis. Antiphospholipid syndrome. Each one had its own Wikipedia rabbit hole, its own constellation of terrifying complications, its own online support groups filled with people sharing horror stories. The medical terminology was dense and overwhelming—words like 'granulomatous inflammation' and 'endothelial dysfunction' that I had to look up just to understand the explanations. What struck me most was how much the symptoms overlapped. Headaches could be any of them. Vision problems could be any of them. Fatigue, brain fog, weird neurological symptoms—they were all on every single list. I started making a spreadsheet because that's what I do when I'm anxious, trying to map which symptoms pointed to which diagnosis. But the more I researched, the more confused I became. One forum post would say 'this is definitely Behçet's,' and the next person with identical symptoms would have vasculitis. How were doctors supposed to figure this out if patients with the same problems had completely different diseases? Every condition had overlapping symptoms with everything else, and I started to wonder if my body had just decided to rebel against itself entirely.
 Image by RM AI
Image by RM AI
The Vision Test That Changed
Dr. Martinez wasn't even supposed to be part of this anymore—I'd been transferred to neurology and rheumatology—but Dr. Chen had asked him to do one more visual field test while we waited for the autoimmune results. 'Just to establish a baseline,' she'd said, which I now understood was doctor-speak for 'we're worried about this.' The test was the same as before: click the button when you see the flash of light, stare at the central point, don't move your eyes. But this time, something felt different. The flashes on the edges weren't as bright. Or maybe they weren't there at all? I kept second-guessing myself, wondering if I was clicking too late or if the machine was broken. When Dr. Martinez pulled up the results next to my previous test from two weeks ago, his expression changed. The colored map of my visual field showed more dark spots—areas where the light hadn't registered. He was quiet for a long moment, then called Dr. Chen right there from the exam room. I couldn't see the dots on the edges anymore, and Dr. Martinez said quietly, 'We're running out of time.'
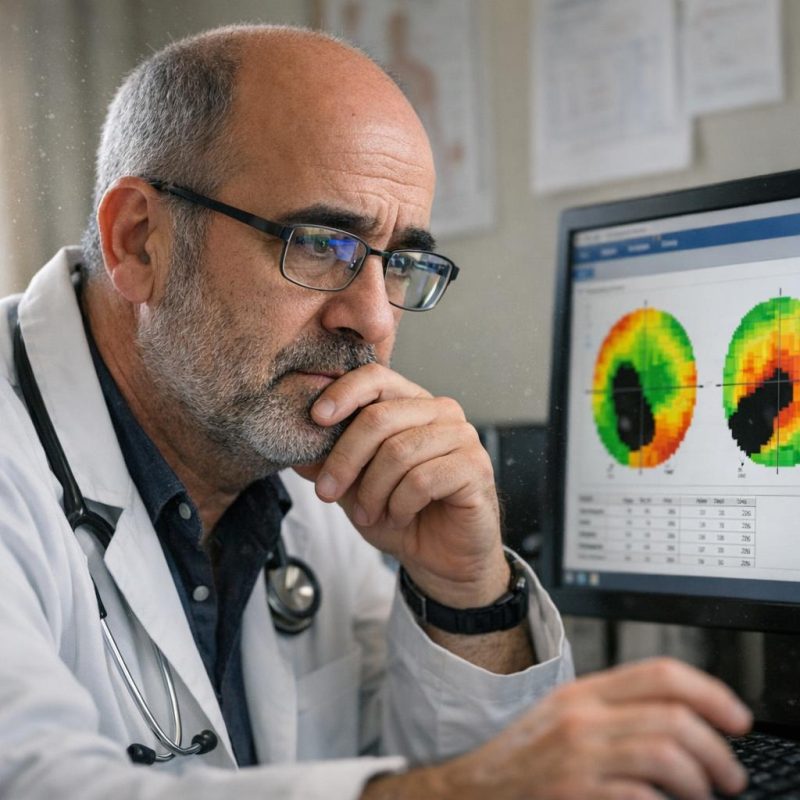 Image by RM AI
Image by RM AI
The Emergency Protocol
Dr. Chen saw me the next morning. Not in two weeks when the full autoimmune panel would be back, not next week for a follow-up—the next morning. That's when I knew things had shifted from concerning to critical. She had Dr. Martinez's visual field results on her screen, and she didn't waste time on pleasantries. 'Your peripheral vision is deteriorating,' she said. 'If this continues, the damage could become permanent. We can't wait for a definitive diagnosis anymore.' She explained that while we didn't know exactly which autoimmune condition was causing the pressure, we knew my immune system was involved based on the preliminary bloodwork. And we knew my optic nerves were being compressed. The plan was aggressive: high-dose corticosteroids to reduce inflammation immediately, plus a medication to reduce cerebrospinal fluid production. 'We're treating the mechanism even though we don't have the full picture yet,' she said. 'Sometimes you have to stop the damage before you fully understand what's causing it.' I signed consent forms for medications with side effect lists that terrified me almost as much as losing my vision. She said we couldn't wait anymore for a diagnosis—we had to treat the symptoms before I lost any more vision, even if we didn't know the cause yet.
 Image by RM AI
Image by RM AI
Lisa's Question
Lisa came over the day I started the steroids. She brought soup and bread and sat with me while I dealt with the first wave of side effects—jittery energy, racing heart, a weird metallic taste in everything. We were talking about the treatment plan when she asked, out of nowhere, 'Do you ever blame yourself for this?' The question hit me harder than I expected. 'What do you mean?' I said, even though I knew exactly what she meant. 'Like, wondering if you caused it somehow. If you stressed too much or didn't take care of yourself enough or ignored symptoms too long.' She was looking at me with this gentle, knowing expression. 'Because I did that when I was sick. Spent so much energy wondering what I did wrong.' I opened my mouth to say no, of course not, this wasn't my fault. But the words stuck in my throat. Because wasn't I always wondering that? Every time a doctor had dismissed me, hadn't I left thinking maybe I was overreacting? Maybe I was being dramatic? Maybe if I'd pushed harder sooner, or eaten better, or rested more, this wouldn't be happening? I said no, but we both knew I was lying—I'd been wondering what I did wrong since the first symptom appeared.
 Image by RM AI
Image by RM AI
The Antibody Results
The first batch of autoimmune results came back while I was still adjusting to the steroid dose. Dr. Chen called me to come in rather than discussing over the phone, which I'd learned was never a good sign. When I got there, she had printouts of lab values spread across her desk, numbers highlighted in yellow and pink. 'Your ANA is positive,' she said, pointing to one value. 'And you have elevated inflammatory markers—ESR and CRP are both high. We're also seeing some unusual antibody patterns that don't fit neatly into any single diagnosis.' She walked me through each result, explaining what it meant and what it didn't mean. The positive ANA suggested autoimmune activity, but lots of people had positive ANAs without disease. The inflammatory markers confirmed something was definitely wrong, but didn't tell us what. The antibody patterns were the most frustrating—present enough to be significant, but not matching the classic presentations of lupus or Sjögren's or any of the other conditions they'd tested for. 'Think of it this way,' Dr. Chen said. 'We know your immune system is confused and causing inflammation. We just don't know yet which specific autoimmune condition is driving it.' Dr. Chen said my immune system was definitely confused about something, but the tests weren't giving us the clean answer we needed.
 Image by RM AI
Image by RM AI
The Night Before Answers
The final results would be ready tomorrow. Dr. Chen had called to schedule an appointment, and she'd used that specific tone doctors have when they actually have something to tell you, not just another 'let's wait and see.' James took the day off work to come with me. We didn't talk much that evening—what was there to say? I'd been in medical limbo for so long that the idea of actually having an answer felt surreal. Part of me had started to believe this would go on forever, that I'd just be the woman with the mysterious symptoms and the growing list of specialists who couldn't quite figure it out. I kept thinking about all the chapters that had led here. The cancelled eye exam. Dr. Martinez's face when he saw my optic nerves. The ER visits and the brain scans and the spinal tap. The three-page document of dismissed symptoms. Every test, every appointment, every moment of being told it was anxiety or stress or just life. All of it was about to be recontextualized by whatever Dr. Chen said tomorrow. I tried to imagine feeling relieved, validated, scared, angry—but mostly I felt numb. Tomorrow I would finally know what was wrong with me, and I couldn't decide if not knowing had been harder than whatever I was about to learn.
 Image by RM AI
Image by RM AI
The Diagnosis I Never Expected
Dr. Chen had both Dr. Martinez and a rheumatologist I'd never met in the room when James and I arrived. That's when I knew this was it—the real answer, not another maybe or let's investigate further. 'We have a diagnosis,' Dr. Chen said, and I felt James reach for my hand. 'You have an autoimmune condition causing idiopathic intracranial hypertension. Essentially, your immune system is triggering inflammation that affects how your body produces and absorbs cerebrospinal fluid, creating the pressure we've been seeing.' She pulled up images, charts, test results. 'This explains everything—the headaches you've had for years, the whooshing sound, the vision changes, all of it. This condition can fluctuate, which is why your symptoms came and went. And it's often missed or misdiagnosed because the symptoms overlap with so many other things.' The rheumatologist added, 'The autoimmune component is what makes your case unusual. Most IIH cases aren't immune-mediated, but yours is. That's why the standard approach wasn't working.' I felt something crack open inside my chest. Every dismissed symptom, every time I'd been told it was stress or anxiety, every appointment where I'd left feeling crazy—it had all been this. She said, 'All those times doctors told you it was anxiety—you were right to know something was wrong. Your immune system has been attacking you for years,' and suddenly every dismissed symptom made horrible sense.
 Image by RM AI
Image by RM AI
Rewriting My History
I went home and pulled out every medical record I'd kept over the past ten years. Sat at my kitchen table with them spread out like evidence at a crime scene. That headache in 2015 that lasted three weeks—I'd been told it was stress from work. The whooshing sound I first noticed in 2017—they said it was probably nothing, maybe earwax. The fatigue that came and went, the weird visual disturbances I'd described as 'sparkles' because I didn't have better words, the neck pain, the dizziness. Every single symptom was documented. Every single one had been dismissed. I had emails where I'd asked for referrals and been told to try meditation instead. Notes from appointments where doctors wrote 'patient anxious' and 'recommends therapy.' One actually wrote 'likely psychosomatic' right there in my chart. And now I knew—they were all wrong. Not just wrong, but dangerously wrong. The autoimmune condition had been attacking me for years, building pressure in my skull, damaging my optic nerves, and I'd been begging people to help me while they patted my hand and suggested yoga. Every headache, every moment of fatigue, every time I felt crazy for complaining—it was all this disease, and I'd spent years being told it was all in my head.
 Image by RM AI
Image by RM AI
The Treatment That Should Have Started Years Ago
Dr. Chen walked us through the treatment protocol like she was reading a manual that should have been opened years ago. 'We'll start with immunosuppressive therapy to calm the autoimmune response,' she said. 'High-dose corticosteroids initially, then we'll transition to longer-term immune modulators. We'll also use medication to reduce CSF production while your system stabilizes.' She showed us studies, success rates, timelines. 'Most patients respond well to this combination. We should see improvement within weeks, significant changes within months.' James asked the question I couldn't. 'If she'd been diagnosed earlier—' Dr. Chen didn't flinch. 'If we'd caught this three years ago, or even two, we likely could have prevented the optic nerve damage entirely. The vision loss, the severity of symptoms—much of it was preventable with proper treatment.' I felt something shift in my chest. Not just anger, though that was there. Something darker, heavier. 'This was always treatable?' I asked. She nodded. 'Yes. The medications have been available for decades.' She said this was treatable—had always been treatable—and I had to leave the room because I couldn't process what that meant for all the time I'd lost.
 Image by RM AI
Image by RM AI
Fighting for My Vision
The infusion center became my second home. They started the immunosuppressive protocol the following Monday, and I sat in a recliner with an IV in my arm while the medication dripped slowly into my bloodstream. Rachel, the nurse who'd been so kind during my lumbar puncture, was assigned to my case. 'You're going to feel like crap for a few days,' she told me honestly. 'But we're buying your vision time to heal, if it's going to.' That 'if' hung there between us. Dr. Chen had been clear—we didn't know how much damage was reversible. Some optic nerve injury was permanent. We were racing against a clock that might have already run out. The medication made me nauseated and shaky. My hands trembled. I got mouth sores and headaches—different headaches, the kind that came from treatment instead of disease, and I learned to tell the difference. But I showed up for every infusion, every appointment, every blood test to monitor my crashing immune system. Because what else was I going to do? Give up? Let the disease win after fighting this hard to name it? The first infusion lasted six hours, and every minute I wondered if we'd started in time or if my optic nerves were already too damaged to save.
 Image by RM AI
Image by RM AI
The First Sign of Hope
Two weeks into treatment, Dr. Martinez called me in for another visual field test. I sat in that dark room again, clicking the button every time I saw a dot of light. My hands were sweating. I kept thinking about the last test, about all that black space where my peripheral vision used to be. When he came back with the results, his face was different than I'd ever seen it. 'Karen, look at this.' He pulled up both tests side by side on his computer screen. 'This is two weeks ago. This is today. See the difference?' I saw it. The black areas hadn't shrunk much, but they hadn't grown either. The deterioration had stopped. 'You're stable,' he said, and his voice caught slightly. 'The progression has halted. And here—' he pointed to a few spots along the edge '—we're seeing some early signs of recovery. It's minimal, but it's there.' I couldn't speak. Stable felt like a miracle after months of watching my vision disappear piece by piece. Dr. Martinez said 'stable' like it was a miracle, and I realized we'd stopped the progression—but I didn't know yet if I'd get back what I'd already lost.
 Image by RM AI
Image by RM AI
What I'm Fighting For
That night, I couldn't sleep. I got up and found a notebook—one of those fancy ones you buy with good intentions and never use. I started writing down everything I wanted to see again without fear. James's face in the morning light. The way shadows fall across our garden in summer. My hypothetical future grandchildren, if Sarah ever has kids. Sunsets. The expressions on my students' faces when they finally understand a concept. The spines of books on my shelf. Birds in flight. My own hands doing ordinary things. The list grew. I wrote down mundane things like grocery store aisles and street signs. Beautiful things like art museums and autumn leaves. Silly things like bad TV shows and James doing his terrible dance moves. I filled pages. When I reached a hundred items, I realized something that made my chest tight—I'd been preparing to lose them. For months, maybe years, I'd been unconsciously cataloging what I loved about seeing, like someone taking inventory before a disaster. I'd been saying goodbye without admitting it. I wrote down fifty things, then a hundred, and realized I'd been preparing to lose them without ever fighting to keep them until now.
 Image by RM AI
Image by RM AI
The Pressure Drops
Dr. Patel scheduled another lumbar puncture after four weeks of treatment. I knew the drill by now—the positioning, the pressure, the strange ache. But this time felt different because we were hoping for something instead of just searching. When he measured the opening pressure, I watched his face. He paused. Rechecked his equipment. Measured again. 'Twenty-two,' he said quietly. I blinked. 'Twenty-two?' The last measurement had been thirty-eight. Before that, forty-two. 'Twenty-two centimeters of water,' he confirmed. 'Normal range is typically under twenty-five. You're almost there, Karen.' I started crying before I could stop myself. After months of astronomical pressure crushing my optic nerves, damaging my vision, causing the relentless headaches—I was almost normal. The immunosuppressive therapy was working. My rogue immune system was finally calming down, stopping its attack on my cerebrospinal fluid regulation. 'This is excellent progress,' Dr. Patel said, and I noticed he was smiling. The number was almost normal, and Dr. Patel smiled—actually smiled—and I started to believe I might actually win this fight.
 Image by RM AI
Image by RM AI
Sarah's Confession
Sarah showed up at my house unannounced on a Tuesday evening. She'd been texting more, checking in, but I hadn't seen her in person since early in my diagnosis. She looked older, tired. We sat in my living room with tea neither of us drank. 'I need to tell you something,' she said. 'Watching you go through this—watching you fight to be believed, fight for answers, fight to save your vision—it's terrified me. Not because I don't think you'll be okay. Because I realized I've been ignoring my own health issues for years.' She told me about irregular periods she'd dismissed, fatigue she'd blamed on her job, joint pain she'd learned to live with. 'I've been doing exactly what you did,' she said. 'Telling myself it's normal, it's stress, it's nothing. But seeing what happened to you, how much damage was done while doctors weren't listening—I can't ignore it anymore. I scheduled appointments. I'm getting tested. Because if you hadn't fought this hard, you'd be blind, Karen. And I don't want to wait until something irreversible happens to me.' She said watching me fight made her realize she needed to address her own health issues, and I understood that my struggle had rippled out further than I knew.
 Image by RM AI
Image by RM AI
The Vision That Returned
Six weeks into treatment, Dr. Martinez ran another visual field test. I sat in the dark room, my finger on the button, watching for those dots of light. But this time—this time I saw dots I hadn't seen in months. Little pinpricks at the edges of my vision, in spaces that had been nothing but black void. My heart started racing. I clicked the button faster, worried I was imagining it, that I wanted it so badly I was inventing lights that weren't there. When Dr. Martinez pulled up the comparison, I saw it wasn't my imagination. The black areas had shrunk. Not dramatically—we were talking small improvements, incremental recovery. But the trend line was moving in the right direction. Some of my peripheral vision was coming back. Not all of it. Maybe not even most of it. But enough to prove that early intervention had made a difference, that catching it when we did—even though it felt so late—had saved me from permanent, complete vision loss. I could see the dots on the edge of the screen again—not all of them, but more than last week—and I cried through the entire test.
 Image by RM AI
Image by RM AI
The Appointment I Almost Canceled
During my follow-up with Dr. Chen, she pulled out my file and showed me something that made my blood run cold. The timeline. She traced her finger along the dates—from my first symptoms to that initial eye exam, from Dr. Martinez's referral to my first appointment with her. 'If you'd waited another month,' she said, looking me straight in the eye, 'the damage would have been irreversible. The inflammation was progressing rapidly. Another few weeks, maybe less, and we would have been talking about permanent blindness, not peripheral vision loss.' I sat there staring at her, thinking about all the times I almost didn't make that call. How I'd picked up my phone to cancel the appointment because it seemed like an overreaction. How I'd convinced myself I was being dramatic, that I should just wait and see if it got better on its own. How close I came—how terrifyingly close—to being the version of myself who shrugged it off, who didn't want to bother anyone, who trusted the first dismissal instead of pushing for answers. Dr. Chen said if I'd waited another month, the damage would have been irreversible, and I couldn't stop thinking about the version of me who almost didn't make that call.
 Image by RM AI
Image by RM AI
Building My New Normal
The weird thing about surviving something like this is that life doesn't just go back to normal. You don't get cured and walk away unchanged. I have a chronic autoimmune condition now. That means regular blood work, ongoing immunosuppressants, constant monitoring for flares or new symptoms. James helped me set up a medication schedule, organized my prescriptions into one of those daily pill containers I used to associate with my grandmother. Every morning I take my pills and think about how this is just my life now—not a temporary crisis, but a permanent reality. Some days my vision is better than others. I've learned to recognize the warning signs of inflammation, the subtle changes that mean I need to call Dr. Martinez right away. I can't predict flares, can't control when my immune system decides to attack itself again. But I've learned to manage it, to adapt, to advocate for myself when something feels off. The uncertainty used to terrify me—still does, sometimes. But mostly I've made peace with it. It wasn't the future I'd planned, but I was learning to live with it—and more importantly, I was actually living.
 Image by RM AI
Image by RM AI
Telling My Story
Lisa called me one afternoon with an idea. She'd been thinking about my story, about how many people go through what I went through—symptoms dismissed, time wasted, diagnoses missed. 'You should share this,' she said. 'Publicly. Not just with friends, but with people who need to hear it.' So I started talking about it. I wrote about my experience online, joined autoimmune support groups, spoke at a local health advocacy event about the importance of listening to patients, of taking symptoms seriously even when they seem vague or 'all in your head.' I talked about the doctors who dismissed me and the ones who saved me. About trusting yourself when something feels wrong. About pushing for answers even when you're scared of being difficult or dramatic. People started reaching out—strangers who'd been dealing with unexplained symptoms for months, who'd been told it was stress or aging or nothing at all. Some of them got proper testing because of my story. Some of them caught their conditions early. The first time someone told me my story helped them push for proper testing, I understood why I'd survived this—to make sure others didn't go through what I did.
 Image by RM AI
Image by RM AI
The Call I'm Glad I Made
Looking back now, I can see the whole journey clearly. From that first moment of blurred vision I tried to ignore, through the dismissals and delays, to Dr. Martinez's face changing when he saw what was happening behind my eyes. I think about the Karen who almost canceled that appointment, who almost decided her symptoms weren't worth investigating. She was so close to letting it go, to trusting the first doctor who said nothing was wrong, to accepting that maybe she was just getting older or stressed or making a big deal out of nothing. But I didn't let it go. I made the call. I showed up. I pushed for answers even when it felt uncomfortable, even when I worried I was being difficult. That decision—that simple act of not canceling, of trusting that something was wrong even when I couldn't prove it—saved my vision, my health, and maybe my life. So if you're reading this and something feels off in your body, if doctors are dismissing you but you know deep down that something isn't right—listen to that voice. I almost canceled that appointment. I almost let it go. But I didn't—and that decision saved my vision, my health, and maybe my life. If you feel like something's wrong, trust that feeling. Make the call. Don't wait.
 Image by RM AI
Image by RM AI






